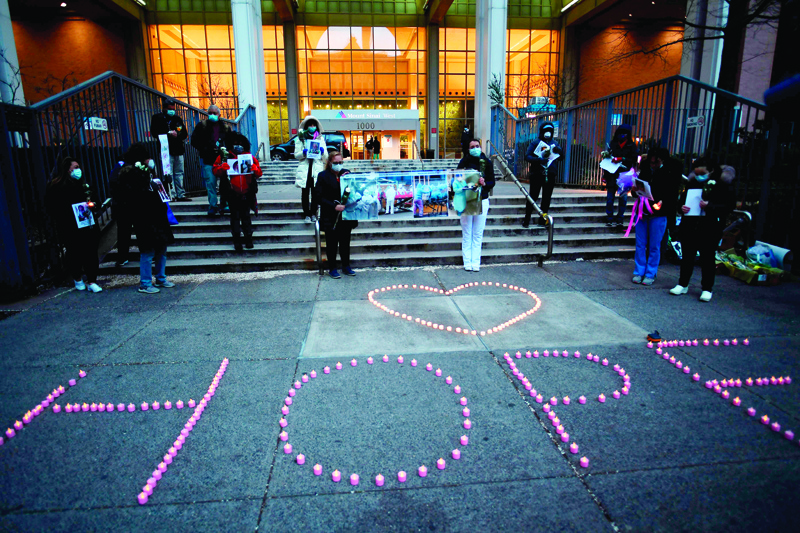
NEW YORK: Unclaimed victims of the new coronavirus are being buried in unmarked mass graves by contract laborers on an island in New York, officials confirmed Friday. Hart Island is one of America's largest public cemeteries, with more than one million people buried there.
New York authorities have used the site for over 150 years to lay to rest unclaimed bodies, unidentified people and residents whose families could not afford a private burial. "We will continue using the island in that fashion during this crisis and it is likely that people who have passed away from COVID who fit this description will be buried on the island in the coming days," a spokesperson for the city government told AFP.
The New York Times reported that around 25 people are being buried on Hart Island a day since the coronavirus crisis started last month. Before the outbreak it was 25 a week. New York has borne the brunt of America's pandemic, registering some 160,000 confirmed cases, more than any country outside of the United States, including Europe's hardest-hit nations of Spain and Italy.
The state's death toll is 7,844, around half of deaths across the US. The mile-long Hart island, which sits in a tidal estuary in the Bronx, became a potter's field in 1869 after the city purchased it from a private landholder to bury unknown and indigent residents. Approximately 1,200 burials take place every year. The dead are placed in pine coffins laid in trenches. There are no gravestones but small white markers indicate the trenches.
The site has long been run by the city's prisons department, and inmates from the nearby Rikers Island, one of America's most notorious jails, are typically paid to perform the burials - although not during the coronavirus pandemic. "We are using contract labor," the spokesperson said. Still-born children and AIDS victims have also been buried on Hart Island over the years. The site was off-limits to the public for decades but in recent years relatives have been allowed to visit on designated days.
Late last year, New York's city council voted to transfer control of Hart Island to its parks department and make it easier for the public to visit. The island has served as a prison camp for captured Confederates in the US Civil War, a mental asylum, a sanatorium for tuberculosis sufferers, a youth detention center and even a Cold War-era missile base. It is often referred to as New York's "island of the dead" or "jail for the dead."
Tributes
Clutching flowers, candles and photos, New York hospital workers paid tribute to colleagues who have died from the coronavirus since the beginning of the epidemic that has ravaged the city with a modest ceremony in the freezing cold Friday. Standing in front of the Mount Sinai Hospital Group in Manhattan, with a heart drawn in electric candles on the sidewalk and letters spelling out the word "HOPE", they made short speeches remembering the nurses, doctors and other hospital workers who fell victim to the virus.
Many clutched photographs of the deceased. "We are here to honor, to pray and remember our fallen heroes," said nurse Joanne Mee Wah Loo to the small group of people who came to pay tribute despite the chill wind. No one knows exactly how many caregivers have died since the beginning of the epidemic in New York City, the most affected metropolis in the US, with nearly 95,000 people infected and more than 5,800 dead.
But was at Mount Sinai that Kious Kelly, the first New York nurse known to die of coronavirus, passed away at the end of March. "He was a good person, a hard worker, he loved what he was doing," says Lenore Leiba, a nurse who knew him and attended this tribute. "It is important to celebrate his life, their lives, and who they really were. They were not worried about their lives, they were thinking of others."
'Inhumane'
Tirzah Caraballo, surgical pathologist secretary at Montefiore Hospital in the Bronx, came to honor Christine Hunt, who died last Sunday after 35 years as a receptionist at the hospital. "She was our mom, our friend, our sister," Caraballo said. "She was denied a mask because she was a secretary. And this is why she's no longer with us."
In the early days of the pandemic, she explained, administrative staff were not allowed masks as they were reserved for nurses and doctors. She acknowledges there are now masks for everyone. "Yes, things have improved since, but we lost so many. It shouldn't have been a decision of who gets a mask and who doesn't. That's inhumane," she said.
The ceremony didn't last long. It began at 7:00 pm, the time when the applause for the caregivers in New York City resounded. A fire truck stopped and several firefighters took the time to applaud, as well as a few passers-by. Forty minutes later, it was over. "Thank you for coming," said Judy Sheridan-Gonzalez, president of the New York State Nurses Association, who attended the ceremony. "We hope we don't have to do this again."
Meanwhile, any premature lifting of restrictions imposed to control the COVID-19 pandemic could lead to a fatal resurgence of the new coronavirus, the World Health Organization warned Friday. WHO chief Tedros Adhanom Ghebreyesus said that while some states were considering ways to ease the restrictions which have placed around half of humanity under some form of lockdown, doing so too quickly could be dangerous.
"I know that some countries are already planning the transition out of stay-at-home restrictions. WHO wants to see restrictions lifted as much as anyone," he told a virtual press conference in Geneva. "At the same time, lifting restrictions too quickly could lead to a deadly resurgence. The way down can be as dangerous as the way up if not managed properly. "WHO is working with affected countries on strategies for gradually and safely easing restrictions."
Tedros spelled out six factors that should be considered before restrictions could be safely eased. He said that transmission would have to be controlled; sufficient public health services made available; outbreak risks in care homes minimized; preventative measures imposed in workplaces and schools; virus importation risks managed; and communities made aware of and engaged in the transition.
Africa acceleration
The global death toll has gone over 100,000. More than 1.6 million infections have been recorded globally, according to an AFP tally, since the virus first emerged in China in December. Tedros welcomed signs that its spread was slowing in some of the hardest-hit countries in Europe - citing Spain, Italy, Germany and France. But he also warned of an "alarming acceleration" of the virus elsewhere, highlighting Africa, where he said it was beginning to emerge in rural areas.
"We are now seeing clusters of cases and community spread in more than 16 countries" on the continent, the former Ethiopian health minister said. "We anticipate severe hardship for already overstretched health systems, particularly in rural areas, which normally lack the resources of those in cities." Tedros said that even the countries with the world's strongest health systems had been caught by surprise by COVID-19. He urged them to reinforce their healthcare provision rather than plunge into a "cycle of panic and neglect".
In many countries, "we're now in a phase of panic because there is this dangerous, invisible virus which is wreaking havoc," he said. "But that should actually lead into asking questions on what to do to strengthen our system. "No country is immune."
Exit strategy
The WHO director-general also said he was particularly concerned by the large numbers of cases being recorded among health workers - with more than 10 percent reportedly infected in some nations. "When health workers are at risk, we're all at risk," he said. Tedros said evidence from some countries, including China, Italy and the United States, showed that health workers were being infected outside healthcare facilities, in their homes and communities.
Switching to the Ebola outbreak in the Democratic Republic of the Congo, he said a new case had been reported, just three days before a deadline that would have marked the official end to the long epidemic. WHO emergencies director Michael Ryan said some 2,600 alerts were still being investigated every day in the DRC, with thousands of samples taken every week. "Maybe that's our lesson for COVID-19: there is no exit strategy until you're in control of the situation, and you must always be ready to go back again and start again," he said. - AFP











